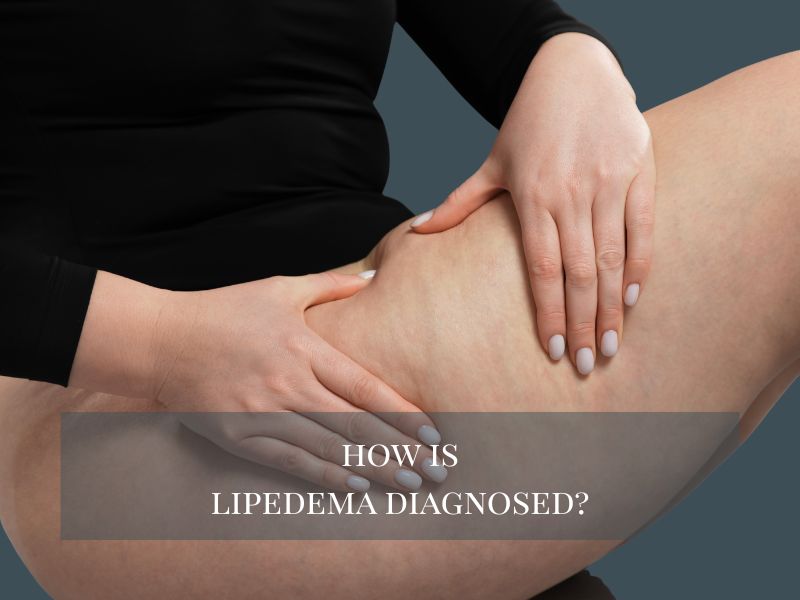
Many people who notice persistent swelling or an unusual buildup of fat in their legs eventually start asking the same question: how is lipedema diagnosed? In the beginning, it often looks very similar to normal weight gain. Because of this, some patients spend years trying different diets, exercise plans, or lifestyle changes without seeing improvement in the affected areas. Understanding how the lipedema diagnosis process works can help patients recognize the signs earlier and seek the right medical evaluation.
Lipedema is a chronic condition that causes an abnormal accumulation of fat, most commonly in the lower body and sometimes in the arms. Since the symptoms can resemble other conditions, doctors usually rely on a combination of medical history, a careful physical examination, and clinical experience to diagnose lipedema. During a consultation with Dr. CV Chegireddy at Aesthera Plastic Surgery, patients can receive a thorough evaluation and guidance on the next steps, helping determine the most appropriate treatment plan for managing lipedema.
Table of Contents
ToggleWhat Is Lipedema?

Lipedema is a condition involving unusual growth of fat tissue beneath the skin. These lipedema fat deposits tend to appear around the hips, thighs, and legs, and in some cases they affect the arms as well. Unlike typical weight gain, the fat accumulation linked to lipedema usually develops body equally on both sides.
The disorder affects the body’s adipose tissue differently from standard fat storage. Many patients notice that their upper body remains fairly proportional while the lower body becomes heavier over time.
Several characteristics help distinguish lipedema from other types of excess fat:
- Symmetrical swollen legs
- Tender or painful fatty tissue
- Easy bruising due to fragile blood vessels
- Fat that does not respond to weight loss
The exact cause of lipedema is still unclear. However, specialists frequently observe that symptoms begin around periods of significant hormonal changes, such as puberty, pregnancy, or menopause. A strong family history is also common among lipedema patients, suggesting that genetics may contribute to the condition.
Why Getting an Accurate Lipedema Diagnosis Matters
Getting a proper diagnosis early can make a meaningful difference in long-term outcomes and daily comfort. When lipedema is mistaken for normal weight gain or obesity, patients often spend years attempting lifestyle changes that do little to affect the underlying lipedema fat.
Over time, the condition may worsen. As lipedema progresses, the tissues may begin holding more fluid and pressure can build in the affected areas.
When lipedema goes untreated, complications may develop such as:
- Increased fluid accumulation
- Persistent fluid swelling
- Development of secondary lymphedema
- Reduced mobility
- Ongoing discomfort in affected areas
Eventually the lymphatic system can become overloaded. When drainage slows down, fluid buildup may appear in the tissues, leading to a more advanced stage known as lipo lymphedema.
The good news is that an early diagnosis allows patients to begin treatments that help manage swelling, improve mobility, and protect overall health. Depending on the patient, care may include compression therapy, physical therapy, lifestyle guidance, or procedures designed to remove fat associated with lipedema.
Who Diagnoses Lipedema?
A trained healthcare provider familiar with lymphatic or vascular disorders typically performs a lipedema diagnosis. Because the condition can resemble several other disorders, experience with lipedema is important.
Specialists who may evaluate patients include:
- Vascular medicine physicians
- Dermatologists
- Plastic surgeons
- Lymphatic disorder specialists
- Specialized physical therapists
Sometimes diagnosis involves more than one professional. For example, a physician may perform the initial assessment while a physical therapist evaluates mobility, swelling, and lymphatic flow.
Working with providers who understand how the lymph vessels and lymphatic system function can help ensure the condition is properly recognized.
Lipedema: How Is It Diagnosed?
So, practically speaking, how is lipedema diagnosed in a clinic or consultation setting? Doctors usually follow several steps: reviewing symptoms, examining the body, and occasionally using imaging or other diagnostic tests.
Unlike many diseases, there isn’t a single lab result that confirms lipedema. Instead, physicians rely on patterns seen during evaluation to reach a clinical diagnosis.
Reviewing Medical History and Symptoms
The process usually begins with a detailed review of the patient’s medical history.
During this conversation, the doctor asks about:
- When lipedema symptoms first appeared
- Whether symptoms began after hormonal changes
- Any family history of similar fat distribution
- Previous attempts at weight loss
- Pain or tenderness within the fat tissue
Many patients describe trying to lose weight through exercise and diet while their legs remain unchanged. Even when they maintain a healthy weight, the fat accumulation in the lower body often persists.
Other commonly reported experiences include:
- Easy bruising
- Sensitivity in the fatty tissue
- A feeling of heaviness in the legs
- Occasional flu like symptoms
- These details help doctors determine whether the pattern matches lipedema fat deposits rather than ordinary fat.
Physical Examination of Fat Distribution
A careful physical examination plays a central role in lipedema diagnosis.
During the physical exam, the physician observes how fat is distributed across the body. Lipedema tends to follow a recognizable pattern.
Typical findings may include:
- Symmetrical enlargement of the hips and thighs
- Fat extending from the hips toward the ankles
- A visible difference between upper body and lower body
The doctor may also gently examine the underlying tissue with their hands to evaluate consistency and tenderness.
Checking for Symmetry and Pain Sensitivity
Another important step involves assessing symmetry.
Lipedema almost always affects both sides of the body equally. Doctors compare the right and left sides of the legs to look for this pattern.
They also test for pain sensitivity. When pressure is applied to the fat tissue, some patients experience discomfort that wouldn’t normally occur with ordinary fat.
In certain cases, even patients with mild symptoms report noticeable tenderness in the affected areas.
Evaluating Skin Texture and Tissue Changes
During the physical exam, doctors also look at the skin surface and the feel of the tissues underneath.
In early stages, the skin may appear smooth while the fat cells underneath begin forming small nodules. As the condition progresses, the fat accumulation may create a slightly uneven or nodular texture.
Changes in the underlying tissue often help doctors determine how far the condition has developed.
Assessing Swelling and Bruising Tendencies
Another part of the lipedema diagnosis process involves evaluating swelling patterns and bruising.
Unlike classic lymphedema, swelling in lipedema tends to remain symmetrical. Doctors also check whether patients bruise easily.
Possible signs include:
- Visible fluid buildup
- Sensitivity when pressure is applied
- Easy bruising due to fragile blood vessels
Because the small vessels in lipedema-affected fat tissue can be delicate, bruises sometimes appear even after minor contact.
Common Signs Doctors Look for During a Lipedema Diagnosis
When evaluating a patient, physicians often look for patterns that are strongly associated with lipedema.
Disproportionate Fat in the Legs or Arms
One of the most recognizable symptoms of lipedema is disproportion between the upper and lower body.
Many patients have a relatively typical body above the waist while the hips and legs become enlarged. In some cases, lipedema also affects sometimes arms.
Fat That Does Not Respond to Diet or Exercise
Another defining feature is fat that remains unchanged despite lifestyle changes.
Some lipedema patients maintain an active routine and stable healthy weight, yet the lipedema fat in the legs remains. This happens because the disorder involves abnormal fat cells, not typical fat storage.
Painful or Tender Fat Tissue
Pain is another important clue.
Many patients report that the lipedema fat deposits feel sore when pressed. This tenderness in the fat tissue may increase gradually as lipedema progresses.
Easy Bruising in Affected Areas
Fragile blood vessels often cause easy bruising.
Patients sometimes notice bruises appearing without clear injury. Doctors often consider this pattern when forming a clinical diagnosis.
Feet and Hands Typically Spared
A distinctive feature of lipedema is that swelling usually stops at the ankles or wrists.
The feet and hands often remain unaffected, which helps doctors distinguish lipedema from secondary lymphedema and other causes of fluid swelling.
Conditions That Can Be Confused With Lipedema
Several conditions can resemble lipedema, which is why careful evaluation is important.
Lipedema vs. Lymphedema
Both conditions involve swelling, but they arise for different reasons.
Lymphedema develops when the lymphatic system cannot properly drain fluid, leading to fluid accumulation in the tissues.
Lipedema, however, primarily involves abnormal fat accumulation. In some patients, long-standing lipedema eventually disrupts lymphatic flow, which may lead to secondary lymphedema.
Lipedema vs. Obesity
Obesity typically involves generalized weight gain and increased adipose tissue throughout the body.
In contrast, lipedema causes specific abnormal fat deposits in the lower half of the body. Even after significant weight loss, the lipedema fat often remains.
Lipedema vs. Lipohypertrophy
Lipohypertrophy also involves enlarged fat tissue, but the symptoms differ.
Unlike lipedema, lipohypertrophy does not cause pain, bruising, or fluid swelling, which helps physicians distinguish the conditions during evaluation.
Are There Tests to Confirm Lipedema?
Lipedema is primarily considered a clinical diagnosis, but doctors sometimes order diagnostic tests to better understand symptoms or rule out other disorders.
Imaging Tests (Ultrasound or MRI)
Ultrasound or MRI may help doctors examine the structure of fat tissue and surrounding tissues.
These scans can reveal changes in the underlying tissue and may also detect fluid buildup.
Lymphatic System Evaluation
If a provider suspects involvement of the lymphatic system, specialized imaging may evaluate lymph vessels and lymphatic flow.
This helps determine whether the patient has developed secondary lymphedema or progressed to lipo lymphedema.
Blood Tests to Rule Out Other Conditions
Although blood tests do not confirm lipedema, they may help rule out other causes of swelling, including chronic venous insufficiency or metabolic disorders.
Lipedema Stages and Classification
Doctors categorize lipedema into stages to describe how far the condition has progressed.
Stage 1 Lipedema
In stage 1, the skin surface appears smooth while small nodules develop within the fat cells beneath the skin.
Patients may experience mild symptoms, including tenderness or easy bruising.
Stage 2 Lipedema
At stage 2, the fat accumulation becomes more visible and uneven. The skin may appear slightly irregular as fat deposits enlarge.
Swelling and discomfort often increase during this stage.
Stage 3 Lipedema
Stage 3 involves larger masses of fat tissue, which can significantly change body contour.
At this stage, mobility may be affected as the expanding fatty tissue places pressure on surrounding structures.
Stage 4 Lipedema (Lipo-Lymphedema)
The most advanced stage occurs when the condition begins affecting the lymphatic system.
This stage, known as lipo lymphedema, involves both abnormal fat and increased fluid accumulation, leading to severe swelling.
When to See a Specialist for Lipedema Evaluation
People who experience persistent swollen legs, tenderness in fat tissue, or unusual fat distribution should consider consulting a specialist.
Seeking evaluation becomes especially important when symptoms begin after significant hormonal changes or gradually worsen over time.
Treatment strategies often aim to effectively manage symptoms and may include:
- Compression garments or compression stockings
- Manual lymphatic drainage
- Compression therapy
- Specialized physical therapy
These approaches support lymphatic flow, help manage swelling, and protect the function of the lymphatic system.
Lipedema Diagnosis and Next Steps for Treatment
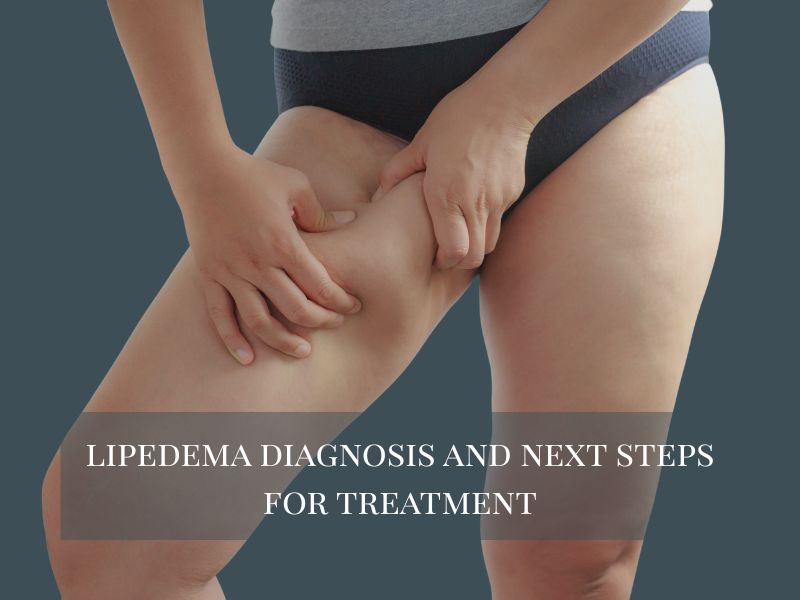
Once a lipedema diagnosis is confirmed, the next step is developing a personalized treatment plan.
Management usually depends on the stage of the condition, symptom severity, and the patient’s overall health.
Many treatment plans include:
- Compression garments to improve circulation
- Manual lymphatic drainage to encourage fluid movement
- Targeted physical therapy with a trained physical therapist
- Lifestyle strategies for maintaining a healthy weight
In some cases, surgical options may help remove fat associated with lipedema. Liposuction techniques designed for treating lipedema can reduce excess fat, relieve pressure on surrounding tissues, and improve mobility.
Research in this area continues to evolve, and some patients may qualify for clinical trials studying new approaches to care.
Although lipedema is a chronic condition, early identification and treatment can help patients reduce pain, maintain mobility, and improve their long-term quality of life.
FAQs
What is the best way to diagnose lipedema?
Doctors usually diagnose lipedema through a combination of symptom review, medical history, and a detailed physical examination. Because there is no single test that confirms the condition, physicians rely on patterns like symmetrical abnormal fat deposits, pain in the fat tissue, and persistent swelling to make a clinical diagnosis.
Can lipedema be detected through medical tests?
Most of the time lipedema is identified clinically rather than through one specific test. Imaging studies like ultrasound or MRI may still be helpful. These diagnostic tests allow doctors to look at the structure of fat tissue and check the lymphatic system if secondary lymphedema is suspected.
What symptoms help doctors identify lipedema?
Doctors often look for several typical lipedema symptoms, including symmetrical swollen legs, tenderness in the fat tissue, and easy bruising. Another important clue is fat that does not respond to weight loss efforts. When the feet remain unaffected while the legs enlarge, it further supports a lipedema diagnosis.
Does lipedema get worse over time?
Yes, in many cases lipedema progresses gradually. Over time the fat accumulation may increase and the tissues may begin holding more fluid. When the lymphatic system becomes affected, some patients develop lipo lymphedema, which leads to more severe swelling.
Can lipedema be treated after diagnosis?
While there is no cure for lipedema, several options help patients effectively manage symptoms. Treatments may include compression therapy, manual lymphatic drainage, physical therapy, and sometimes procedures designed to remove fat linked to lipedema. These strategies can improve comfort and protect long-term mobility.
How can you recognize an early stage lipedema stomach?
In the early stages, lipedema in the stomach may present as a gradual, even buildup of soft fat in the abdominal area that feels different from typical weight gain. Patients often notice tenderness, a feeling of heaviness, or skin that bruises more easily. Because it doesn’t improve significantly with diet or exercise, a proper evaluation is important to confirm the diagnosis and discuss appropriate management options.
Book Your Lipedema Consultation
Living with lipedema can affect comfort, mobility, and confidence. At Aesthera Plastic Surgery by Dr. CV Chegireddy, patients can receive a detailed evaluation and learn about available options for lipedema treatment. A consultation allows the doctor to assess your symptoms, review your goals, and recommend a personalized treatment plan.
Book your consultation today to take the next step toward managing lipedema and improving your quality of life.