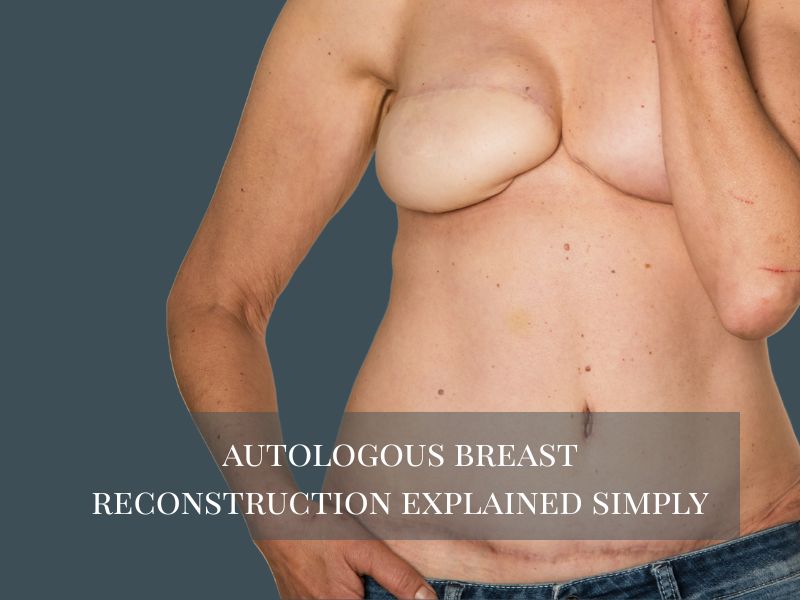
At Aesthera Plastic Surgery by Dr. CV Chegireddy, Autologous Breast Reconstruction is one of the most advanced and natural options available for women undergoing breast reconstruction after breast cancer treatment. As part of the journey through mastectomy surgery, many patients explore breast reconstruction surgery to restore the breast area and regain a sense of wholeness.
With guidance from experienced plastic surgeons like Dr. CV Chegireddy, patients can choose from a wide range of reconstruction approaches, including breast implants, flap surgery, and several advanced autologous reconstruction techniques.
Table of Contents
ToggleIntroduction to Breast Cancer and Reconstruction

For many women, breast cancer treatment involves mastectomy surgery, which can significantly alter the appearance of the chest. Breast reconstruction offers an opportunity to restore the breast tissue, shape, and volume through either breast implants or autologous breast reconstruction.
According to data from the National Cancer Institute, hundreds of thousands of women are diagnosed with breast cancer each year in the United States. As a result, access to quality reconstruction surgery has become an integral part of modern cancer care.
Patients may choose:
- Breast implants (saline or silicone)
- Autologous reconstruction, using skin and fat, blood vessels, and sometimes muscle
- Hybrid approaches combining implants with acellular dermal matrix
- Delayed or immediate reconstruction after cancer treatment or radiation therapy
Consultation with a qualified breast reconstruction plastic surgeon ensures patients understand which option best meets their medical needs, aesthetic goals, and long-term plans.
Types of Reconstruction
Implant Reconstruction
Implant reconstruction is one of the most common options following mastectomy. This method involves placing breast implants, which can be saline, silicone, or textured implants, beneath the chest muscle or directly under the skin. In many cases, surgeons use acellular dermal matrix to provide additional support, help shape the breast, and improve overall results. This approach is often chosen by women who prefer a simpler, shorter procedure or who are not candidates for flap-based reconstruction.
One of the main advantages of implant reconstruction is the shorter surgical procedure, which makes it appealing for women looking for a less complex option. Recovery is typically smoother and faster compared to flap procedures, allowing patients to return to daily activities more quickly. Another benefit is the ability to adjust size with a permanent implant, giving women the opportunity to achieve the breast shape and volume that fits their preferences and body proportions.
Autologous Reconstruction
Autologous breast reconstruction uses the patient’s own tissue to rebuild the breast, creating a soft, warm, and natural-feeling reconstructed breast. Because the tissue comes from your own body, this method offers the most realistic look and feel. It is especially helpful after radiation therapy, which can sometimes complicate implant reconstruction. Many women choose autologous reconstruction because it blends naturally with the rest of the body and provides long-lasting, comfortable results.
There are several ways to perform autologous reconstruction, depending on where the tissue is taken from and how it is transferred. Free flaps, which require microsurgery, allow surgeons to completely disconnect the tissue and reconnect it to new blood vessels in the chest. Pedicle flaps, which remain partially attached to donor site blood vessels, keep some of the original blood supply intact during the transfer. The tissue can come from different areas of the body, including the abdomen, back, buttock, or inner thigh, depending on what is best for the patient’s body type and goals.
Flap Surgery Options
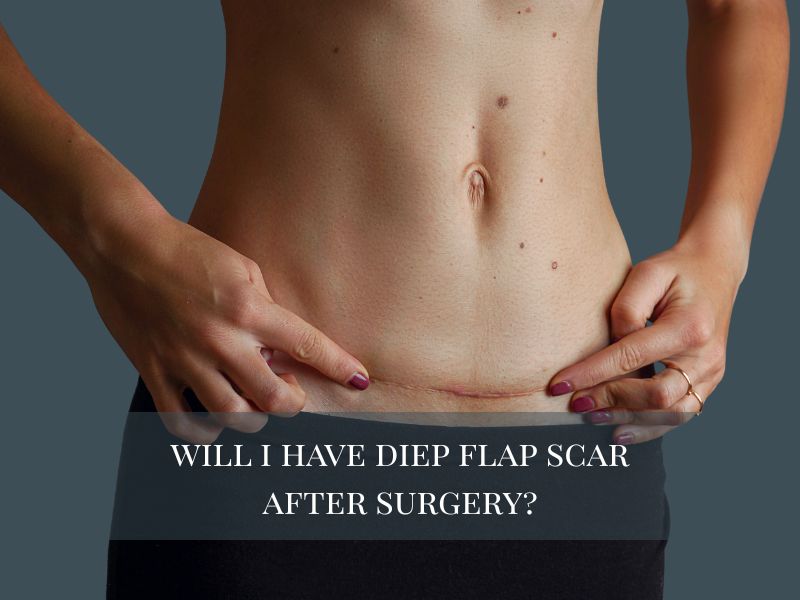
DIEP Flap Surgery
The diep flap (short for deep inferior epigastric perforator) is one of the most advanced and preferred forms of flap breast reconstruction. During diep flap surgery, the plastic surgeon transfers skin and fat—but not abdominal muscles—from the lower abdomen to the chest.
Benefits of the diep flap procedure:
- Preserves the abdominal muscle
- Creates a natural, soft new breast
- Offers long-term durability
- Improves abdominal contour, similar to a tummy-tuck effect
TRAM Flap Surgery
TRAM flap surgery (transverse rectus abdominis myocutaneous flap) uses abdominal tissue but may involve sometimes muscle. Options include:
- Pedicle TRAM flap
- Free TRAM flap
Although effective, TRAM flaps vs DIEP flap may weaken the abdominal wall compared to the DIEP method.
Latissimus Dorsi Flap
The latissimus dorsi flap uses skin fat and sometimes muscle from the back. This approach is ideal when the abdomen is not an option or when additional coverage is needed over breast implants.
Thigh-Based Flaps
For patients without enough tissue in the abdomen, thigh-based flaps offer alternatives:
- Vertical upper gracilis flap (VUG flap)
- TUG flap
- PAP flap (profunda artery perforator flap)
- Flaps from the upper inner thigh or the upper thigh
These provide natural volume for a smaller breast mound using donor tissue from the leg.
Free Flap Reconstruction
Free flap surgery involves completely disconnecting the donor tissue, then reconnecting tiny blood vessels using microsurgery. This ensures proper blood supply to the reconstructed area.
Common free flap options include:
- DIEP flap
- SIEA flap (using the superficial inferior epigastric artery)
- Free TRAM flap
- Latissimus dorsi free flap variants
- PAP flap
Key advantages:
- Greater precision
- Ability to sculpt a natural breast
- Reduced long-term complications
- Flexible donor site selection
Autologous Tissue Transfer
Autologous tissue transfer offers unmatched natural results by using autologous tissue, the patient’s own skin, fat, and blood vessels, to reconstruct the breast. This approach is favored by many because it avoids issues related to silicone implants, traditional implants, and the risk of capsular contracture.
Benefits of Breast Reconstruction
Physical and Emotional Benefits:
Autologous Breast Reconstruction offers meaningful physical and emotional benefits for women after mastectomy. One of the biggest advantages is the restoration of the breast area after mastectomy, which helps patients feel whole again. Many women also experience improved confidence and body image, especially when their clothes fit more comfortably and naturally. This procedure allows patients to wear clothing comfortably without extra padding or external prosthetics. Most importantly, it brings a sense of restored normalcy after cancer treatment, helping women reconnect with their bodies and move forward with greater comfort and self-esteem.
Benefits of Autologous Reconstruction:
Choosing autologous reconstruction comes with several long-term advantages. Because the tissue comes from your own body, the results have a natural feel and appearance, which many women prefer. Another benefit is that there is no risk of implant rupture, making autologous Breast Reconstruction a low-maintenance and durable option. It also provides long-lasting results that age naturally with the rest of the body. This approach is compatible with radiation therapy, making it a strong choice for women who need or previously had radiation as part of their cancer treatment. Additionally, autologous reconstruction offers better symmetry for women with unilateral mastectomy, creating a more balanced, natural-looking outcome.
Postoperative Healing and Recovery
Recovery timelines vary depending on the type of reconstructive surgery performed.
General recovery insights:
- Healing may take several weeks to months
- Patients should avoid heavy lifting or strenuous exercise
- Drains typically remain until excess fluid resolves
- Scars soften and fade with time
- Proper wound care reduces the risk of infection or flap necrosis
- Follow-up appointments help ensure a smooth recovery
For flap procedures, the donor site (abdomen, thigh, or back) also requires healing and protection.
Nipple Reconstruction
As a final step in the reconstruction journey, nipple reconstruction helps complete the appearance of the new breast. This phase focuses on restoring a natural-looking nipple and areola, giving the reconstructed breast a more balanced and realistic look. Several approaches can be used depending on the patient’s needs and surgical plan.
One option is surgical nipple creation, where the surgeon forms a small projection using the patient’s own skin. Another method is 3D nipple tattooing, which creates the look of a nipple and areola through detailed shading and color work. In some cases, skin graft techniques are used to achieve the desired texture and shape. For many women who undergo flap procedures, delayed reconstruction several months later may be recommended to allow the tissues to settle and heal properly.
A skilled plastic surgeon will evaluate the patient’s anatomy, healing progress, and personal preferences to determine the most natural and appropriate method. This final step often brings a renewed sense of completeness and confidence for women completing their breast reconstruction journey.
Ideal Candidates for Reconstruction

Patients may be ideal candidates if they:
- Have undergone mastectomy
- Desire a natural-feeling breast mound
- Have sufficient donor tissue for an autologous flap
- Have received or will undergo radiation therapy
- Prefer a reconstructive result using own tissue
FAQs About Autologous Breast Reconstruction
What is autologous breast reconstruction?
Autologous breast reconstruction uses a patient’s own tissue, such as skin, fat, and blood vessels, to recreate the breast after mastectomy surgery. This method provides a natural look and feel, avoids complications linked to breast implants, and is ideal for women who have undergone radiation therapy.
What is the cost of breast reconstruction?
The cost of breast reconstruction can vary depending on the type of procedure, hospital fees, anesthesia, and the surgeon’s experience. Autologous procedures may cost more than implant-based reconstruction because they are longer and more complex. It’s always best to request a full cost breakdown during your consultation so you understand everything included.
Does insurance cover breast reconstruction?
Most insurance plans do cover breast reconstruction after mastectomy, including follow-up revisions when medically necessary. Coverage can vary, so it’s important for patients to review their insurance policies carefully and contact their insurance provider directly for confirmation.
Can I need a revision after breast reconstruction?
Yes, some patients may need a revision after breast reconstruction. A revision can address changes in breast shape, symmetry adjustments, implant issues, or scar improvements. Revisions are common and can help refine the final result so the breasts look and feel more natural over time.
How many stages are involved in breast reconstruction?
The number of stages in breast reconstruction depends on the technique used. Some surgeries can be completed in one stage, while others involve multiple steps, such as the initial reconstruction, nipple reconstruction, and final refinements. Your surgeon will explain your specific roadmap based on your anatomy, healing timeline, and reconstruction method.
Who is a good candidate for autologous reconstruction?
Ideal candidates are women with enough donor tissue, who have completed or will undergo breast cancer treatment, and who desire long-term natural results. Patients who experienced complications with implants or received radiation therapy may also benefit.
Schedule Your Breast Reconstruction Consultation
If you’re considering Breast Reconstruction, the next step is to schedule a personalized consultation at Aesthera Plastic Surgery with Dr. CV Chegireddy.
During your visit, Dr. CV Chegireddy will evaluate your medical history, discuss your reconstruction goals, and recommend the safest and most effective approach for your needs. Our team is here to guide you through every stage of the process and help you feel confident as you move forward with your treatment.